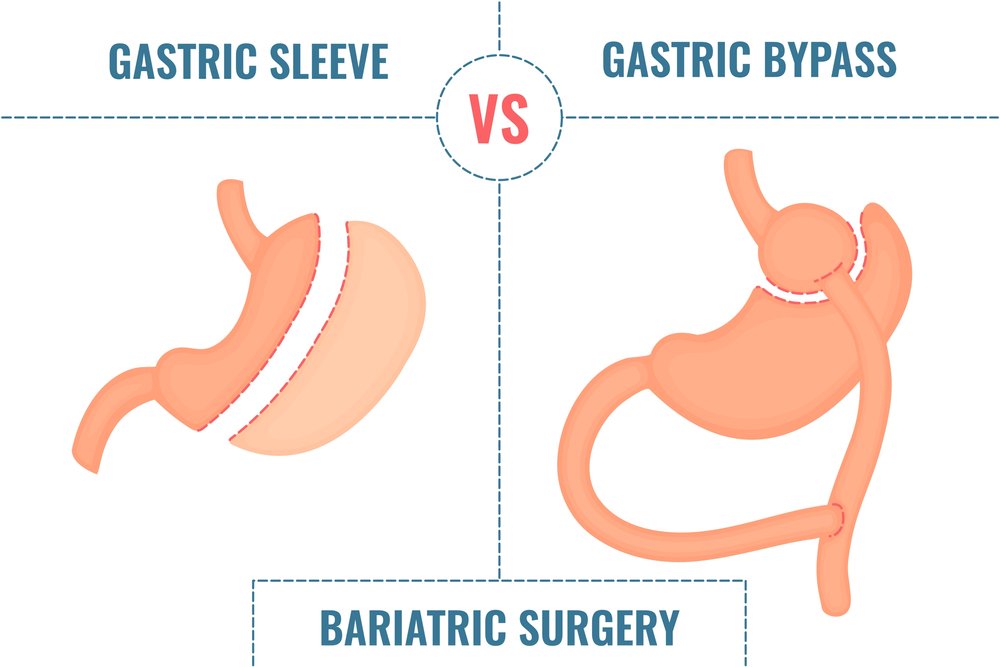
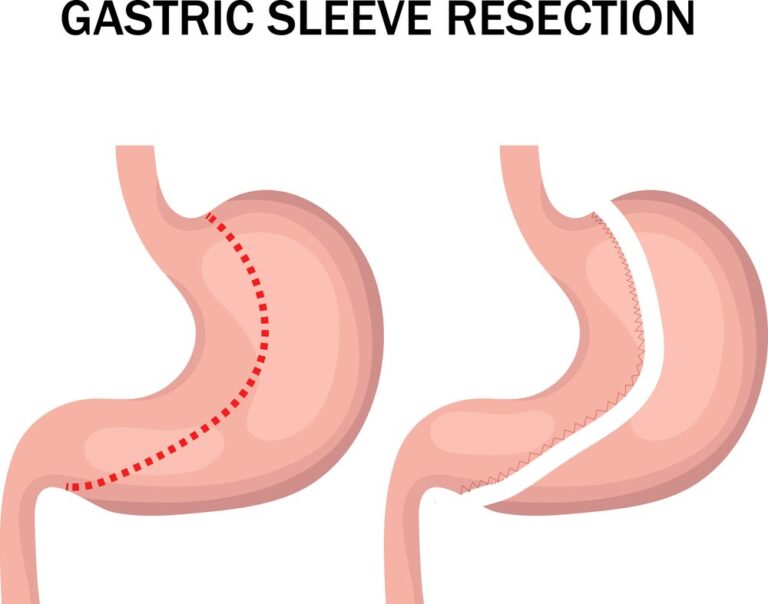
When considering weight loss surgery options, it’s important to weigh the pros and cons of each procedure. Here’s a comparison of the pros and cons of gastric sleeve surgery and gastric bypass surgery:
| Gastric Sleeve Surgery | Gastric Bypass Surgery | |
|---|---|---|
| Pros | – Effective weight loss (60-70% excess weight loss) | – Significant weight loss (60-80% excess weight loss) |
| – Simplified digestive system | – Enhanced long-term weight maintenance | |
| – Fewer long-term nutritional requirements | – Resolution/improvement of coexisting conditions | |
| – Lower risk of dumping syndrome | – Strong impact on hunger hormones | |
| – Lower risk of ulcers | ||
| Cons | – Irreversible procedure | – Complex digestive changes |
| – Potential for acid reflux | – Potential for dumping syndrome | |
| – Limited impact on hunger hormones | – Lifelong nutritional supplementation | |
| – Potentially lower weight loss than gastric bypass | – Higher risk of ulcers |
Please note that this table provides a general overview of the pros and cons of gastric sleeve surgery and gastric bypass surgery. The specific outcomes and experiences may vary for each individual. It is important to consult with a healthcare professional to determine the most appropriate procedure for your unique situation.
Get a $1000 Off on Gastric Sleeve in Miami
Benefits and Drawbacks of Gastric Sleeve Surgery
Gastric sleeve surgery, also known as sleeve gastrectomy, is a popular weight loss procedure that offers several benefits. However, it is important to consider the potential drawbacks as well. Here’s an overview of the benefits and drawbacks of gastric sleeve surgery:
Benefits of Gastric Sleeve Surgery:
- Effective Weight Loss: Gastric sleeve surgery has been shown to result in significant weight loss. Patients can expect to lose around 60-70% of their excess weight within the first year after surgery.
- Improvement in Coexisting Conditions: In addition to weight loss, gastric sleeve surgery often leads to improvements in various obesity-related health conditions, such as type 2 diabetes, high blood pressure, sleep apnea, and joint pain.
- Reduced Hunger: The surgery involves removing a large portion of the stomach, including the area responsible for producing the hunger hormone ghrelin. This reduction in ghrelin levels helps decrease appetite and promote a feeling of fullness.
- Simpler Digestive System: Unlike gastric bypass surgery, gastric sleeve surgery does not involve rerouting or bypassing the intestines. This simplifies the digestive process and reduces the risk of certain complications.
- Faster Recovery Time: Gastric sleeve surgery is generally considered to have a shorter recovery period compared to gastric bypass surgery. It typically requires a shorter hospital stay and allows patients to resume their normal activities relatively quickly.
Drawbacks of Gastric Sleeve Surgery:
- Irreversible Procedure: Gastric sleeve surgery permanently removes a large portion of the stomach, making it irreversible. Once the surgery is performed, the stomach cannot be restored to its original size.
- Potential for Acid Reflux: Some patients may experience an increase in acid reflux symptoms after surgery, although it is usually less severe compared to gastric bypass. Medications and lifestyle modifications can help manage this issue.
- Limited Impact on Hunger Hormones: While gastric sleeve surgery reduces the stomach size and removes the ghrelin-producing area, it has a limited impact on other hunger hormones. This may result in slightly less appetite suppression compared to procedures that involve intestinal changes.
- Lack of Long-Term Data: While gastric sleeve surgery has gained popularity in recent years, it is a relatively newer procedure compared to gastric bypass. Long-term data on the effectiveness and safety of gastric sleeve surgery are still being collected.
It’s important to consult with a healthcare professional to discuss your individual circumstances, weight loss goals, and potential risks and benefits of gastric sleeve surgery. They can provide personalized guidance and help you make an informed decision about the most suitable weight loss approach for you.
Non-Reversible: Important Considerations of Gastric Sleeve’s Irreversibility
One important aspect to consider before undergoing gastric sleeve surgery is the non-reversibility of the procedure. Gastric sleeve surgery permanently alters the size and shape of the stomach, which means it cannot be reversed. Here are some key considerations regarding the irreversibility of gastric sleeve surgery:
- Permanent Removal of Stomach Tissue: During gastric sleeve surgery, a large portion of the stomach is permanently removed, leaving behind a smaller sleeve-shaped stomach. This removed tissue cannot be restored, and the stomach cannot regain its original size or shape.
- Lifetime Commitment: Choosing gastric sleeve surgery requires a lifelong commitment to the changes it brings. Once the procedure is performed, the altered stomach size and capacity will remain for the rest of your life. It’s essential to be mentally prepared for this permanent change.
- Limited Options for Revision: Unlike some other weight loss procedures, such as gastric banding, gastric sleeve surgery does not provide the option for simple adjustments or reversals. If you encounter complications or unsatisfactory results, the options for revision or reversal may be more limited.
- Risks of Secondary Procedures: If you experience complications or unsatisfactory weight loss outcomes after gastric sleeve surgery, secondary procedures may be required. These subsequent surgeries come with their own risks and considerations, and they may be more complex than the initial procedure.
- Evaluation of Long-Term Goals: Before opting for gastric sleeve surgery, it is crucial to evaluate your long-term goals and consider whether the irreversibility aligns with your weight loss objectives. Take into account factors such as expected weight loss, health improvements, and potential impact on your lifestyle.
- Comprehensive Preoperative Assessment: Your healthcare team will conduct a thorough preoperative assessment to ensure that gastric sleeve surgery is the most appropriate choice for you. This assessment will involve evaluating your overall health, discussing your weight loss goals, and exploring alternative options if necessary.
Factors to Consider When Choosing Between Gastric Sleeve and Gastric Bypass
Choosing the right weight loss surgery is a significant decision that should be based on individual needs and considerations. When deciding between gastric sleeve and gastric bypass, several factors should be taken into account. Here are some key factors to consider:
- Weight Loss Goals: Consider your weight loss goals and expectations. Gastric bypass surgery tends to result in slightly greater weight loss compared to gastric sleeve surgery. If you have a higher BMI or desire more aggressive weight loss, gastric bypass may be a better option.
- Health Conditions: Evaluate any existing health conditions you have, such as type 2 diabetes, high blood pressure, or sleep apnea. Gastric bypass surgery has been found to have a greater impact on resolving or improving these conditions compared to gastric sleeve surgery.
- Surgical Approach: Assess your comfort level with the surgical approach of each procedure. Gastric sleeve surgery involves removing a portion of the stomach, while gastric bypass involves rerouting the intestines. Discuss the surgical techniques with your healthcare provider to determine which one aligns better with your preferences.
- Nutritional Considerations: Understand the long-term nutritional requirements of each procedure. Gastric bypass may require lifelong vitamin and mineral supplementation due to the rerouting of the digestive system, while gastric sleeve surgery typically has fewer long-term nutritional requirements.
- Risk Profile: Evaluate the potential risks and complications associated with each procedure. Both surgeries carry risks, and it’s important to discuss them with your healthcare provider. Consider your overall health, medical history, and risk tolerance when assessing the risk profile.
- Recovery and Lifestyle Impact: Consider the impact on recovery and lifestyle changes required after each procedure. Gastric sleeve surgery generally has a shorter recovery period, while gastric bypass may require more significant dietary and lifestyle modifications due to the intestinal changes involved.
- Individual Preferences: Take into account your personal preferences and comfort level with each procedure. Discuss your concerns, expectations, and lifestyle factors with your healthcare provider to ensure the procedure aligns well with your individual circumstances.
Ultimately, the decision between gastric sleeve and gastric bypass should be made in consultation with a qualified healthcare provider who can assess your medical history, perform a comprehensive evaluation, and provide personalized recommendations based on your specific needs and goals.
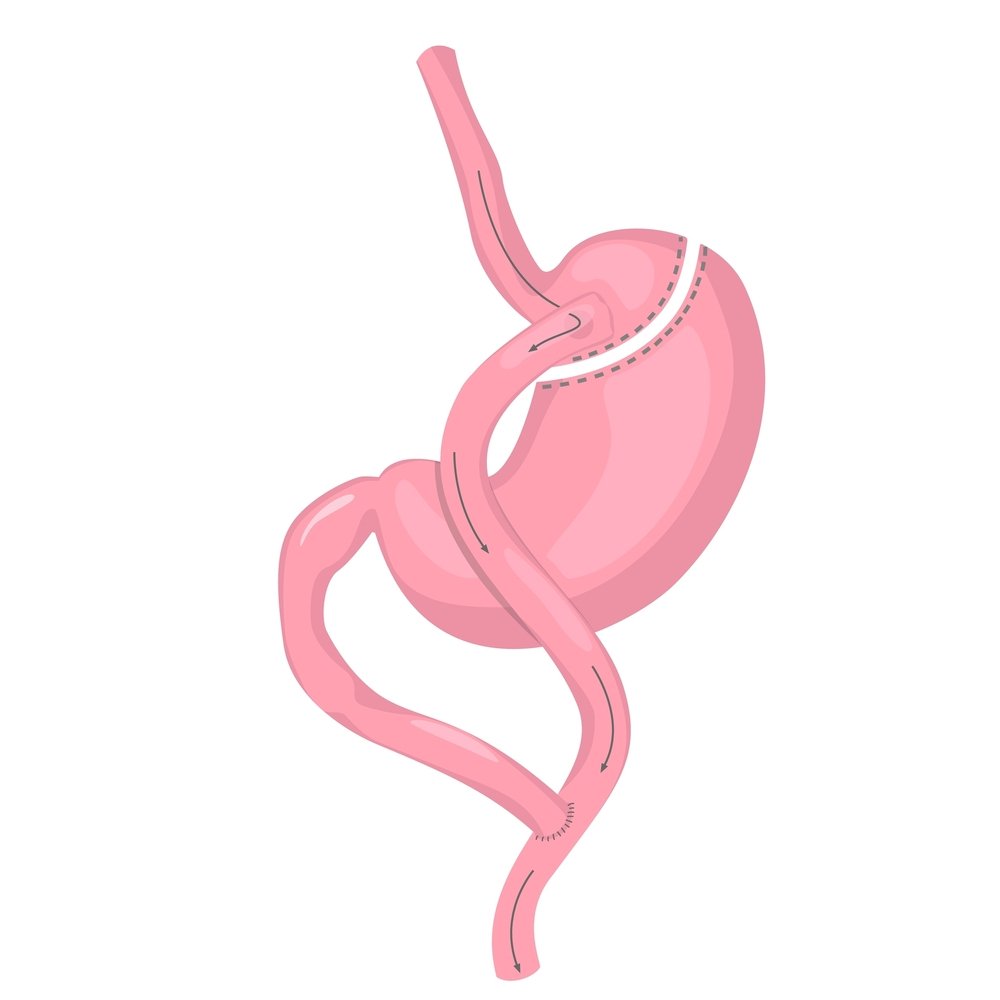
Effective Weight Loss: How Much Can Be Lost with Gastric Sleeve and Gastric Bypass?
Here’s an overview of the weight loss expectations for gastric sleeve and gastric bypass:
| Gastric Sleeve Surgery | Gastric Bypass Surgery | |
| Average Weight Loss | 60-70% of excess weight within the first year | 60-80% of excess weight within the first year |
| Example | If 100 pounds of excess weight: 60-70 pounds | If 100 pounds of excess weight: 60-80 pounds |
| within the first year | within the first year | |
| Factors Influencing Outcome | Age, initial weight, overall health, | Age, initial weight, overall health, |
| adherence to guidelines, physical activity | adherence to guidelines, physical activity |
Please note that these numbers are averages, and individual weight loss outcomes can vary. It’s important to consult with a healthcare provider to discuss your specific circumstances and expected weight loss outcomes based on your unique situation.
Appetite Reduction: How Gastric Sleeve Helps Control Hunger
Gastric sleeve surgery, also known as sleeve gastrectomy, can effectively help control hunger and reduce appetite. The procedure works by altering the size and shape of the stomach, leading to several mechanisms that aid in appetite reduction. Here’s how gastric sleeve surgery helps control hunger:
- Reduced Stomach Size: During gastric sleeve surgery, a large portion of the stomach is permanently removed, leaving behind a smaller sleeve-shaped stomach. This smaller stomach has a reduced capacity to hold food, resulting in a feeling of fullness with smaller portions. The limited stomach space helps control hunger by physically restricting the amount of food that can be consumed.
- Ghrelin Hormone Regulation: The portion of the stomach that is removed during gastric sleeve surgery is responsible for producing the hunger hormone ghrelin. By reducing the size of the stomach, the surgery leads to a decrease in ghrelin production. Ghrelin is a hormone that stimulates appetite and promotes hunger sensations. With lower ghrelin levels, individuals experience reduced feelings of hunger and increased satiety.
- Hormonal Changes: Gastric sleeve surgery triggers hormonal changes beyond ghrelin regulation. The alteration of the stomach’s anatomy affects the release of various hormones involved in appetite regulation, such as peptide YY (PYY), glucagon-like peptide-1 (GLP-1), and insulin. These hormones help promote feelings of fullness, suppress appetite, and regulate blood sugar levels.
- Improved Satiety: With a smaller stomach size and hormone regulation, gastric sleeve surgery enhances the feeling of fullness after meals. Patients find that they are satisfied with smaller portions of food, which helps in reducing caloric intake and promoting weight loss. The improved satiety and reduced appetite make it easier to adhere to a lower-calorie diet, facilitating long-term weight management.
It’s important to note that while gastric sleeve surgery can help control hunger, it does not completely eliminate the desire to eat or address emotional eating habits. Adhering to post-operative dietary guidelines, adopting healthy eating habits, and making lifestyle changes are essential for long-term success in managing hunger and achieving weight loss goals.
Malabsorption Benefits: Why the Malabsorptive Component of Gastric Bypass Is Important
Gastric bypass surgery is a weight loss procedure that combines both restrictive and malabsorptive components. While the restrictive aspect involves reducing the stomach size, the malabsorptive component alters the digestive system to promote weight loss. Here are the reasons why the malabsorptive component of gastric bypass is important:
- Enhanced Weight Loss: The malabsorptive component of gastric bypass plays a crucial role in achieving significant weight loss. By rerouting a portion of the small intestine, the surgery reduces the amount of calories and nutrients that can be absorbed by the body. This results in enhanced weight loss compared to procedures that rely solely on restriction.
- Calorie Reduction: The rerouting of the small intestine bypasses a portion of it, limiting the contact between food and the digestive enzymes and bile. As a result, fewer calories are absorbed from the food consumed, leading to a reduction in calorie intake. This contributes to weight loss by creating a calorie deficit.
- Improved Satiety and Appetite Control: The malabsorptive component of gastric bypass triggers hormonal changes that affect appetite and satiety. The rerouting of the small intestine alters the release of hormones such as ghrelin, peptide YY (PYY), and glucagon-like peptide-1 (GLP-1). These hormonal changes help control hunger, promote a feeling of fullness, and reduce food cravings.
- Resolution of Obesity-Related Health Conditions: The malabsorptive aspect of gastric bypass surgery has been found to effectively improve or resolve certain obesity-related health conditions, including type 2 diabetes, high blood pressure, and sleep apnea. The combination of weight loss and metabolic changes contributes to the beneficial effects on these conditions.
- Maintenance of Long-Term Weight Loss: The malabsorptive component of gastric bypass enhances the long-term maintenance of weight loss. By reducing the absorption of calories, it helps prevent weight regain and provides sustainable results over time.
Body Mass Index (BMI) and Eligibility: Who Is a Candidate for Each Procedure?
The eligibility criteria for gastric sleeve surgery and gastric bypass surgery are often based on the individual’s Body Mass Index (BMI) and overall health condition. Here’s a general guideline regarding the BMI ranges and eligibility for each procedure:
Gastric Sleeve Surgery:
- Gastric sleeve surgery is typically recommended for individuals with a BMI of 35 or higher, although it may be considered for those with a BMI of 30-34.9 if they have obesity-related health conditions such as diabetes, high blood pressure, or sleep apnea.
- Candidates for gastric sleeve surgery should have a significant amount of excess weight and have not achieved satisfactory weight loss through other non-surgical methods.
Gastric Bypass Surgery:
- Gastric bypass surgery is often recommended for individuals with a higher BMI or those with more severe obesity-related health conditions.
- Candidates for gastric bypass surgery generally have a BMI of 40 or higher. It may also be considered for those with a BMI of 35-39.9 if they have significant obesity-related health issues.
- Gastric bypass surgery may be suitable for individuals who have struggled to lose weight through conventional methods and require a more aggressive approach to weight loss.
It’s important to note that BMI alone is not the only factor considered for eligibility. A comprehensive evaluation by a healthcare professional is necessary to assess overall health, medical history, lifestyle factors, and other individual considerations.
Additionally, certain medical conditions or factors may influence the choice of procedure. For instance, gastric bypass surgery may be recommended for individuals with uncontrolled diabetes due to its potential impact on blood sugar control.